The three most common types of skin cancer are: basal cell carcinoma, squamous cell carcinoma, and malignant melanoma. Anyone can be diagnosed with cancer at any age. Doctors link these forms of cancer to overexposure to the sun. Tanning booths can also increase your risk, as can exposure to radiation or high altitude. Because each type of skin cancer has a different look, it is important to alert your physician if you notice unusual changes in the size and shape of spots, the coloration of your skin or the sensitivity and comfort of your body. Time is of the essence, and when caught early, many forms of skin cancer can be successfully treated.
Pre-cancer
Actinic Keratoses (pre-cancers) are pre-malignances, recognized as rough-surfaced patches on sun-exposed skin, often better felt than seen. They are sometimes tender or sensitive and have a gritty feel, like fine sandpaper. They are usually treated with liquid nitrogen, applied by sprayer or cotton tipped applicator, which produces a blister or scab, destroying the pre-malignant cells. They can also be treated with various prescription topical creams, or photodynamic therapy (BLU-U Blue light treatment). A percentage of actinic keratosis develops into skin cancers (mostly squamous cell carcinomas), so it is important to have them treated.
Basal Cell Carcinoma
Basal Cell Carcinomas are the most common cancers of humankind. Fortunately, they are also the most curable! They virtually never spread to other parts of the body, but can invade deeply and destroy or disfigure the eyes, nose, lips, ear or other body parts. They can be recognized as pearly bumps with fine blood vessels on the surface or as sores that do not heal for more than two weeks. Less common forms of basal cell carcinoma can resemble a scar that appears for no apparent reason or even a rash resembling eczema, psoriasis or ringworm, but which does not respond to appropriate therapy for these conditions. Basal cell carcinoma has also been mistaken for a pimple that doesn’t resolve.
Squamous Cell Carcinoma
Squamous Cell Carcinomas usually are rough-surfaced bumps that extend down into the skin, so if you squeeze the skin, it feels like a lump. One variety, called a Keratoacanthoma, looks like a volcano with a central crater and may be tender as a boil. Squamous Cell Carcinomas usually are only locally destructive, but can have some tendency to spread to local lymph glands (metastasize), especially if they are large (over an inch in diameter), left untreated, or on the lip, ear or central face. Bowens Disease is also called Squamous Cell Carcinoma In Situ, and refers to squamous cell carcinoma confined to the top layer of the skin.
Malignant Melanoma
Malignant melanoma is by far the deadliest form of skin cancer. While it occurs less frequently than the other forms of skin cancer, it is more dangerous because, if not treated quickly, it can spread throughout the entire body, proving fatal.
“A B C D E” Guidelines
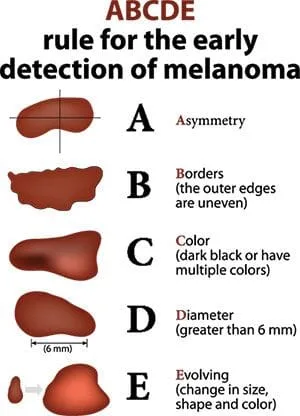
What makes a mole suspicious for melanoma? This has been summarized as the "ABCDE" of melanomas, in which:
- A = Asymmetry of outline
- B = Border irregularity
- C = Color irregularity
- D = Diameter greater than 6 mm (larger than a pencil eraser)
- E = Enlargement of recent origin (or any change)
That is to say that most melanomas are fairly large and irregular in shape and color, while benign moles are generally small and symmetrically round or oval. A rapidly growing, itchy, bleeding or tender mole should arouse suspicion but, conversely, most melanomas produce no symptoms. Things that increase risk include:
- - Two or more blistering sunburns before age 18
- - Fair skin, freckles and sensitivity to the sun
- - Having more than 50 moles
- - Having atypical moles
- - Having a parent, brother, sister or child with a melanoma
- - Having occasional intense sun exposure on weekends or on vacations
If you, a friend or loved one has many moles or a spot that is irregular, a physician should be consulted. If the physician is even slightly suspicious, an almost painless biopsy should be done so the lesion can be examined pathologically. Dozens of moles should be removed for each melanoma found so no melanomas are missed. Even the best dermatologists are only correct 3/4 of the time in diagnosing melanomas by just looking at them! Even if you have no suspicious spots requiring a visit to the dermatologist, you should continue to examine your whole skin once a month using a hand mirror and a full-length wall mirror to better see your back. The sudden appearance of a fairly large, irregularly pigmented flat spot is the most common early sign of a melanoma and should alert you to make an appointment with your doctor. At the same time, as you look at your skin, perform a monthly breast exam if you are a woman or testicle exam if you are a man. This should take a total of five minutes a month or one hour a year - time well spent.
Skin Cancer Diagnosis and Treatment
We recommend that your practitioner biopsy suspicious lesions, rather than aiming to fully remove them at the initial evaluation. As with melanomas, even the most skilled dermatologists are unable to absolutely diagnose skin cancers 100% of the time by eye, and over- and under-treatment can be avoided if a biopsy gives your practitioner the exact diagnoses and an idea of how deep the tumor is growing.
Treatment options for skin cancers include excision (easily performed in our office under local anesthesia), curettement and desiccation, or Mohs micrographic surgery. The latter is a specialized type of excision performed by dermatologists in which the tumor is excised, analyzed microscopically, and mapped, while the patient remains in the office. Mohs micrographic surgery is often used for skin cancers on the face, because it is a tissue sparing surgery with a high cure rate. For a detailed description, please visit www.mohssurgery.org. There are some topical treatments for certain superficial types of skin cancer. We also offer Xoft Electronic Brachytherapy (an isotape-free radiation treatment) as a non-surgical option for select skin cancers. The appropriate treatment depends on skin cancer type, anatomic location of the cancer, and patient and practitioner preferences.
Prevention of skin cancer consists of daily use of sunscreens, protective clothing, and excess sun avoidance. Tanning beds can contribute to skin cancer, and should be absolutely avoided. Regular full body skin examinations help to detect pre-cancers and skin cancers in their earliest stages. Patients are advised to perform a monthly self-skin examination in front of a full length mirror and using a hand held mirror. Any new or non-healing growths should prompt a visit to the dermatologist office. In the future, there may be therapies that can reverse some of the past sun damage done to the skin.